If you have been diagnosed with lichen sclerosus, you know that managing flare-ups is an ongoing effort. While topical steroids remain the cornerstone of treatment, many patients ask whether dietary changes can make a meaningful difference. The relationship between lichen sclerosus diet and symptom management is an evolving area of interest, and at FemRenew in Toronto, Dr. Fay Weisberg encourages patients to consider nutrition as one component of a comprehensive care plan.
The Connection Between Diet and Lichen Sclerosus
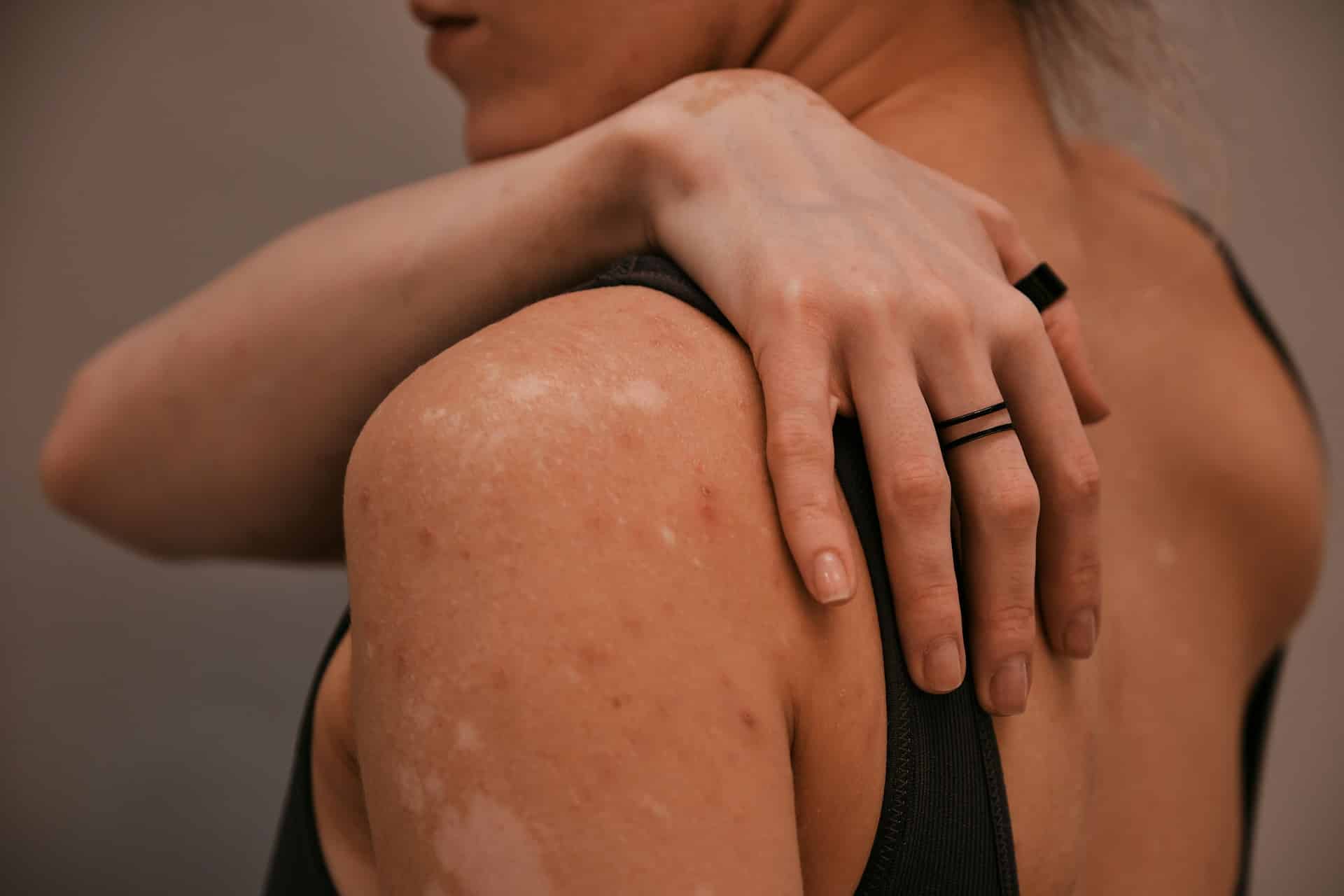
Lichen sclerosus is an inflammatory condition, and inflammation in the body is influenced by many factors — including what you eat. While no specific diet has been clinically proven to cure or prevent lichen sclerosus, research on anti-inflammatory eating patterns suggests that certain foods may help modulate the immune response and reduce the frequency or intensity of flare-ups.
The Harvard Health Publishing outlines how chronic inflammation is linked to diet, noting that specific foods can either promote or reduce inflammatory markers in the body. For a condition driven by immune dysregulation like lichen sclerosus, minimizing inflammatory triggers through diet is a reasonable supportive strategy.
Foods That May Help Manage Lichen Sclerosus Symptoms
An anti-inflammatory dietary approach emphasizes whole, nutrient-dense foods that support immune regulation:
- Fatty fish: Salmon, mackerel, sardines, and herring are rich in omega-3 fatty acids, which have well-documented anti-inflammatory properties. Aim for two to three servings per week.
- Colourful fruits and vegetables: Berries, leafy greens, tomatoes, and bell peppers contain antioxidants and polyphenols that help neutralize inflammatory free radicals.
- Nuts and seeds: Walnuts, flaxseeds, and chia seeds provide additional omega-3s along with vitamin E, which supports skin health.
- Olive oil: Extra virgin olive oil contains oleocanthal, a compound with anti-inflammatory effects comparable to low-dose ibuprofen.
- Turmeric and ginger: Both contain bioactive compounds (curcumin and gingerols, respectively) studied for their ability to reduce inflammatory markers.
- Probiotic-rich foods: Yogurt, kefir, kimchi, and sauerkraut support gut health. An emerging body of research links gut microbiome balance to immune function and autoimmune conditions.
Learn more about the full range of lichen sclerosus treatment options available at FemRenew, including laser therapy and PRP.
Foods That May Worsen Symptoms
Some patients report that certain foods seem to trigger or aggravate their lichen sclerosus symptoms. While individual responses vary, commonly reported dietary triggers include:
- Refined sugars and processed foods: High-sugar diets promote systemic inflammation and may exacerbate immune-driven conditions.
- Gluten: Some lichen sclerosus patients have reported symptom improvement after eliminating gluten, though clinical evidence is limited. If you suspect gluten sensitivity, a supervised elimination trial may be worthwhile.
- Dairy: Certain dairy products can promote inflammation in some individuals, particularly those with lactose intolerance or casein sensitivity.
- Alcohol: Alcohol can increase inflammation and may interfere with immune function. Moderation is advisable.
- Acidic foods: Tomatoes, citrus fruits, and vinegar-based foods can irritate vulvar tissue in some patients, though this is related to direct contact rather than systemic inflammation.
It is important to approach dietary changes methodically. Eliminating multiple food groups simultaneously can be difficult to sustain and may lead to nutritional gaps. Instead, consider removing one suspected trigger at a time for four to six weeks and tracking your symptoms in a journal.
Supplements That May Support Skin Health
In addition to dietary changes, some supplements have shown potential benefits for patients with inflammatory skin conditions:
- Vitamin D: Deficiency is common in patients with autoimmune conditions. Ask your doctor to check your levels and supplement if needed.
- Omega-3 fish oil: If you do not eat fish regularly, a high-quality fish oil supplement (1,000-2,000 mg EPA+DHA daily) may help.
- Probiotics: A daily probiotic with multiple strains can support gut health and immune balance.
- Vitamin E: Applied topically or taken orally, vitamin E supports skin repair. Some patients apply vitamin E oil directly to affected areas as a moisturizer.
Always discuss supplements with your healthcare provider, especially if you take prescription medications, as interactions can occur.
Diet as Part of a Comprehensive Treatment Plan

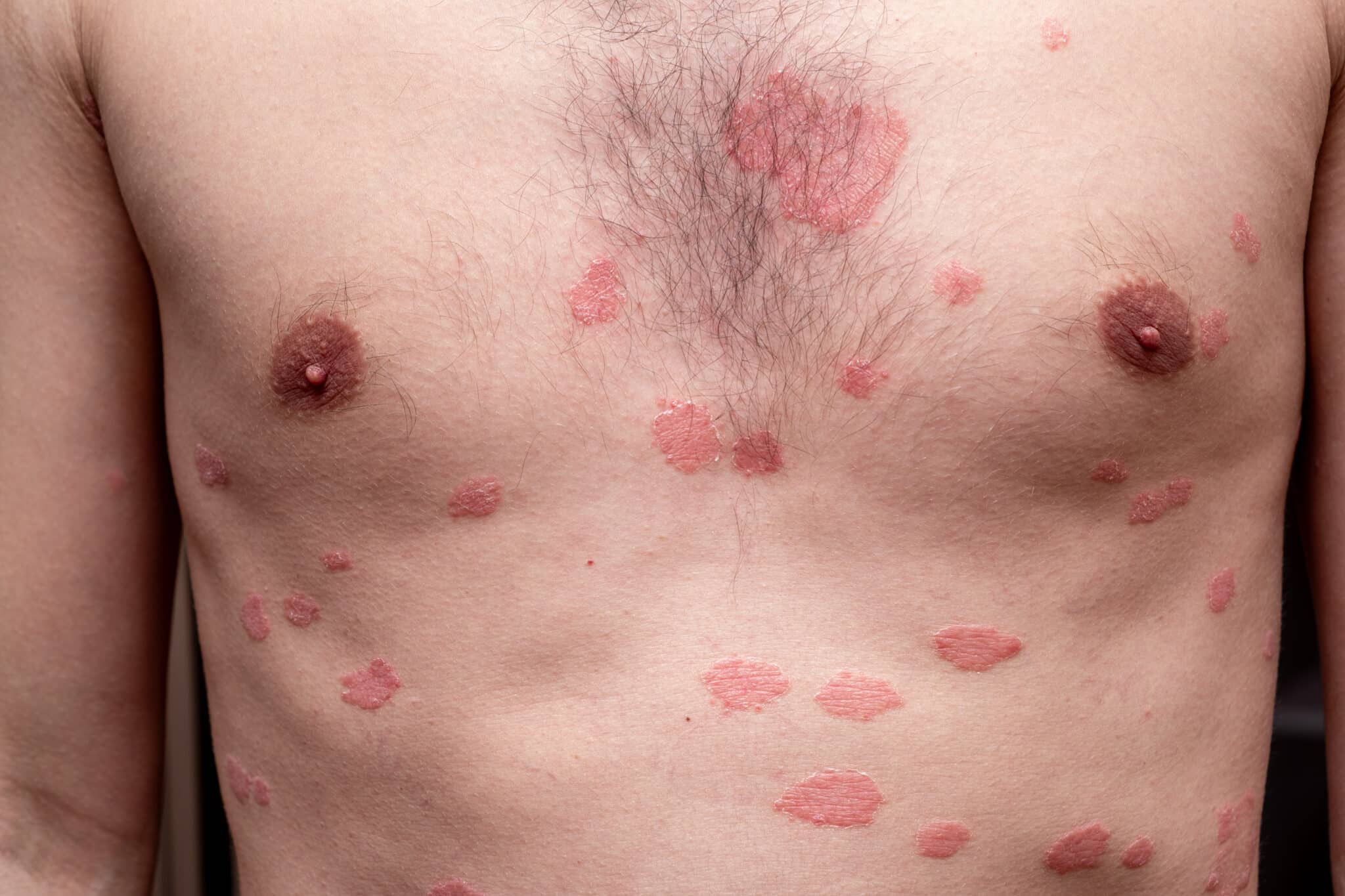
Dietary changes alone are unlikely to control lichen sclerosus symptoms adequately. The most effective approach combines medical treatment — such as topical corticosteroids, laser therapy, or PRP — with supportive lifestyle modifications including diet, stress management, and proper vulvar care.
At FemRenew, Dr. Weisberg takes a holistic view of patient care, recognizing that lasting improvement comes from addressing multiple factors simultaneously. Diet is one piece of the puzzle, not a replacement for proven medical treatments.
Tracking Your Progress with a Food and Symptom Journal
One of the most practical steps you can take is keeping a daily log of what you eat alongside your lichen sclerosus symptoms. Note flare-up severity, itching levels, and any new foods or supplements introduced. After four to six weeks, patterns often emerge that help you and Dr. Weisberg identify which dietary changes are making a measurable difference and which may not be relevant to your specific case.
Frequently Asked Questions
Can diet cure lichen sclerosus?
No. There is currently no cure for lichen sclerosus, and no diet has been proven to eliminate the condition. However, an anti-inflammatory diet may help reduce flare-up frequency and support overall immune health alongside medical treatment.
Should I try a gluten-free diet for lichen sclerosus?
Some patients report improvement after eliminating gluten, but the evidence is anecdotal rather than clinical. If you suspect gluten may be a trigger, try a supervised elimination for four to six weeks and monitor your symptoms carefully before making a permanent change.
What vitamins are good for lichen sclerosus?
Vitamin D, omega-3 fatty acids, vitamin E, and probiotics are the most commonly discussed supplements for patients with lichen sclerosus. Have your vitamin D levels checked, as deficiency is common in autoimmune conditions, and discuss supplementation with your doctor.
Can sugar make lichen sclerosus worse?
Excessive sugar consumption promotes systemic inflammation, which may worsen immune-mediated conditions like lichen sclerosus. Reducing refined sugar intake is a reasonable step that benefits overall health as well.
Get Personalized Guidance at FemRenew
Managing lichen sclerosus effectively requires a multi-faceted approach that includes medical treatment, lifestyle adjustments, and ongoing monitoring. If you want to explore how a lichen sclerosus diet and complementary therapies may fit into your care plan, Dr. Fay Weisberg and the FemRenew team are ready to help. Call (416) 924-4666 or visit our contact page to book your appointment in Toronto.
Medically reviewed by Dr. Fay Weisberg, MD, FRCSC — OB-GYN and Medical Director at FemRenew, Toronto.



